- PATIENT FORMS | REQUEST A CONSULTATION | CONTACT US
- 1-844-NSPC-DOC
Chronic Pain
What Is Chronic Pain?
Take ActionCauses and Symptoms of Chronic Pain
As “pain” is one of the most broadly named symptom of any malady or trauma and has a variety of causes, the diagnosis of it is a complex and multi-phase process, which incorporates a variety of disciplines and diagnostic tests.
Sometimes the cause of pain is identifiable, for example, spinal stenosis or another degenerative disc disease might be causing ongoing pain. Other times, pain sensation from the area where injuries have healed continue to send pain signals.
The most common symptoms of chronic pain are:
- Lasting Physical Pain – Real chronic pain that does not abate after the original injury or illness responsible for it has been dealt with.
- Other Sensations – Some chronic pain symptoms manifest as other sensations, such as burning, dull aches or shooting, electrical pains.
- Muscle Issues – You may experience issues related to muscles and tension, including soreness, stiff joints, limited mobility or tightness.
- Fatigue – One of the more insidious chronic pain symptoms, long-term fatigue can set in when someone endures pain for too long. This can lead to a loss of personal motivation and other psychological complications.
- Insomnia – If you suffer from severe, chronic pain, you may also suffer from insomnia if you are kept up at night by the pain.
- Infection and Illness – Some of the tertiary chronic pain symptoms like fatigue and insomnia can contribute to a weakened immune system, leaving you a prime candidate for developing infection or illness.
- Depression – Perhaps the most severe of the mental chronic pain symptoms that a person can develop, long-term pain can lead to ongoing bouts of depression in some patients.

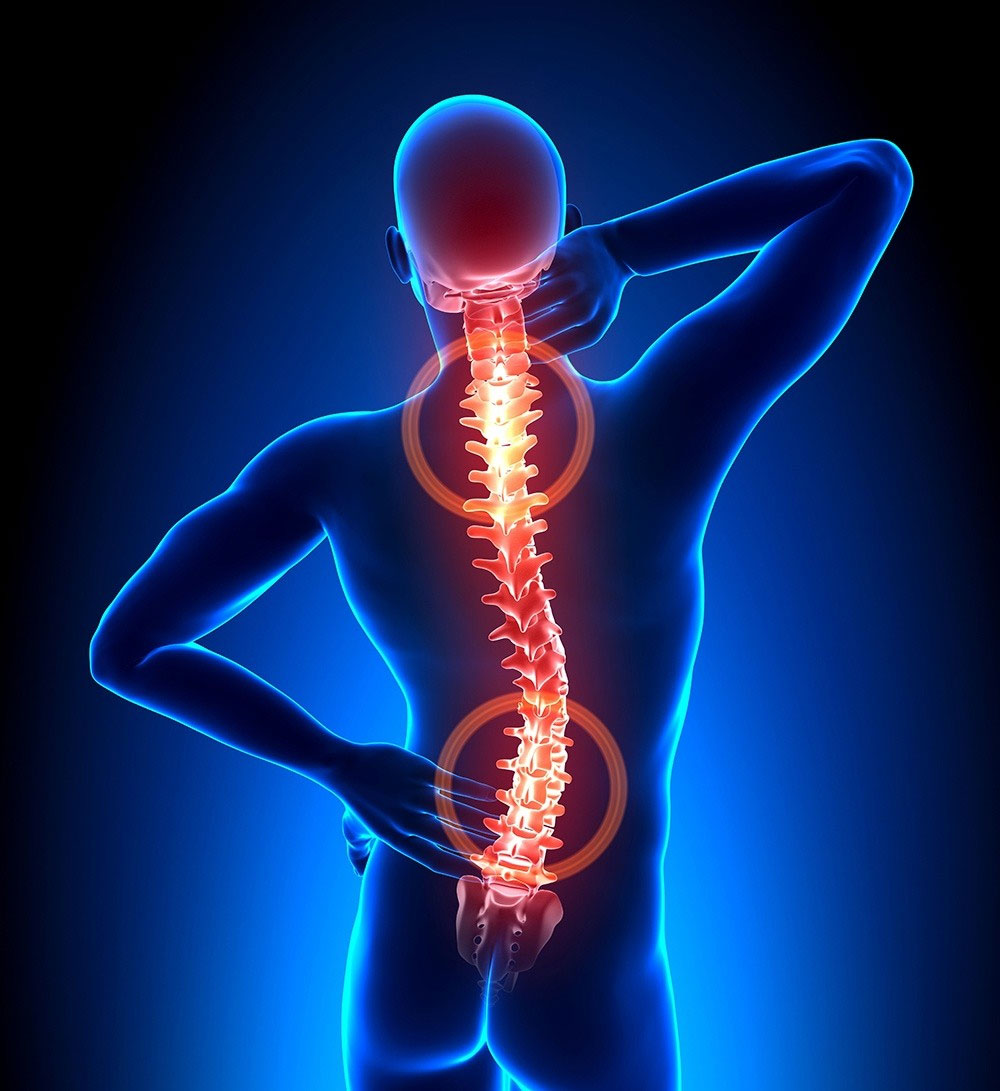
How Is Diagnosis of Chronic Pain Performed?
Whether you are suffering from chronic pain related to your back, head, neck or any other area of your body, the diagnostic process remains basically the same. Despite the best efforts of the medical community, it is hard to quantify pain since it is subjective and tolerance levels differ by individual.
This has led physicians and other medical professionals attempting to perform chronic pain diagnosis to rely on a series of investigative tests in an attempt to identify physical factors that may be causing pain in their patients. Before tests are administered, a physician will typically have a discussion with the patient about the type, frequency and exact location of the pain experienced. Describing pain as sharp rather than dull, constant versus episodic or burning compared to aching can all help the attending physician narrow down possible causes of the pain response.
After the pain history is compiled, chronic pain diagnosis proceeds with imaging tests. X-rays, CT scans, as well as full MRI scans can all be employed in an attempt to isolate factors that may be causing chronic pain. A psychosocial assessment may also be performed; especially if the patient also suffers from depression, fatigue or other mental complications as a result of their chronic pain.
Advanced Treatments for Chronic Pain at NSPC
If you suffer from chronic pain, the team of world-class physicians at Neurological Surgery, P.C (NSPC) in New York will help you through the diagnostic process to determine what form of chronic pain treatment may be best for you:
- Intrathecal drug delivery system implants (an injection of medication directly into the spinal canal via an implant)
- Over-the-counter medication
- Physical therapy
- Alternative therapies
- Injections
- Pharmacologic measures such as narcotics, NSAIDS (non-steroidal anti-inflammatory medicines) and antidepressants
- Neuromodulation (electrical stimulation that interferes with the pain signals to the brain)
Some of the procedures at NSPC regulate the electrical impulses of the nerves to the brain using neuromodulation. Neurostimulation can often provide pain relief when other conservative methods have failed.
Spinal Cord Stimulators
Spinal cord stimulators are minimally invasive treatments that deliver electrical pulses to prevent pain signals from the spinal cord from reaching the brain. As a leader in innovative spine and brain treatments, NSPC offers expert physicians performing cutting-edge procedures for pain management.
Peripheral nerve stimulation is a minimally invasive therapy that involves placing a lead under the skin to stimulate the peripheral nerve fiber network in the area that the pain is located.
Implantable drug pumps deliver medication directly to the intrathecal space (the fluid-filled area surrounding your spinal cord). By introducing the drug directly to your spinal cord, a much smaller dose is required, and this procedure can also be helpful to those who have trouble taking medication orally.
In our New York area practice, we have experienced physicians in the specialties of pain management, critical care neurology, interventional neuroradiology, neuro-oncology, neuro-ophthalmology, epileptology (epilepsy neurology) and neurophysiology, as well as the clinical psychology specialty of neuropsychology to offer top-notch chronic pain management programs along with revolutionary treatment options for depression and other accompanying conditions.
If you have chronic pain related to your back, neck, head or any other area of your body, contact one of our NY metro region medical centers to find out more about our expert chronic pain management treatment options.
Related NSPC Center
Spine Center
Don’t let mobility issues and neck or back pain stop you — NSPC offers exceptional rehabilitation and pain management for your spine disorder. Our team of expert doctors focuses on sophisticated diagnostic techniques, individualized treatment plans, and quality care to help you get your life back, sooner.
Physicians
Connect With Our 7 Convenient Locations
across Long Island, NY
Our expert physicians, surgeons and doctors are ready to serve you at our 7 convenient locations across Long Island, NY. Connect today to learn how our award winning, world class experts can help.
4250 Hempstead Turnpike Suite 4,
Bethpage, NY 11714
(516) 605-2720
COMMACK
353 Veterans Memorial Hwy,
Commack, NY 11725
(631) 864-3900
One Hollow Lane, Suite 212
Lake Success, NY 11042
(516) 442-2250
MANHATTAN
215 E. 77th Street Ground Floor
New York, NY 10075
(646) 809-4719
EAST SETAUKET
226 North Belle Mead Road, Suite C
East Setauket, NY 11733
(631) 828-3001
100 Merrick Road, Suite 128W
Rockville Centre, NY 11570
(516) 255-9031
WEST ISLIP
500 Montauk Hwy
West Islip, NY 11795
(631) 983-8400
World
Class
Expertise
For over 50 years & 350,000 patients NSPC has been a trusted global medical leader.
Contact us today for an appointment or consultation.

