- PATIENT FORMS | REQUEST A CONSULTATION | CONTACT US
- 1-844-NSPC-DOC
Neoplastic Meningitis
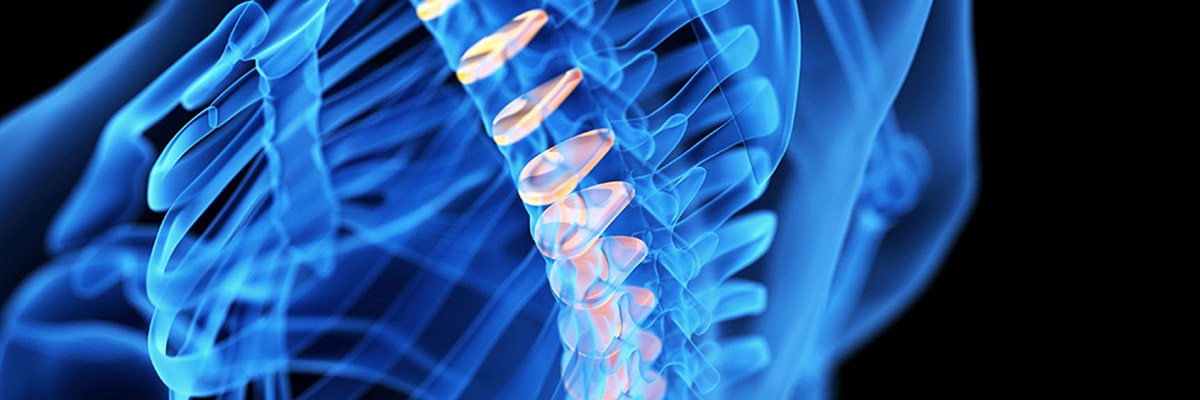
What Is Neoplastic Meningitis?
Take ActionCauses and Symptoms of Neoplastic Meningitis
Since the cerebrospinal fluid is ferrying the cancer cells to the central nervous system—consisting of the brain, spinal nerve roots, and cranial nerves—most of the symptoms relate to cerebral, spinal and cranial nerve dysfunction:
Neoplastic meningitis symptoms in the spinal column can lead to:
- Pain in the neck or back
- Muscle weakness
- Hemiparesis (paralysis on one side of the body)
Cranial nerve dysfunction symptoms, which may be due to increased intracranial pressure, can create cranial nerve palsy:
- Vision problems such as double vision or vision loss
- Tinnitus (ringing in the ears) or hearing loss
- Facial numbness (if the trigeminal nerve is affected)
Cerebral symptoms:
- Headache
- Confusion or mental impairment
- Dizziness
- Seizures
- Nausea and/or vomiting
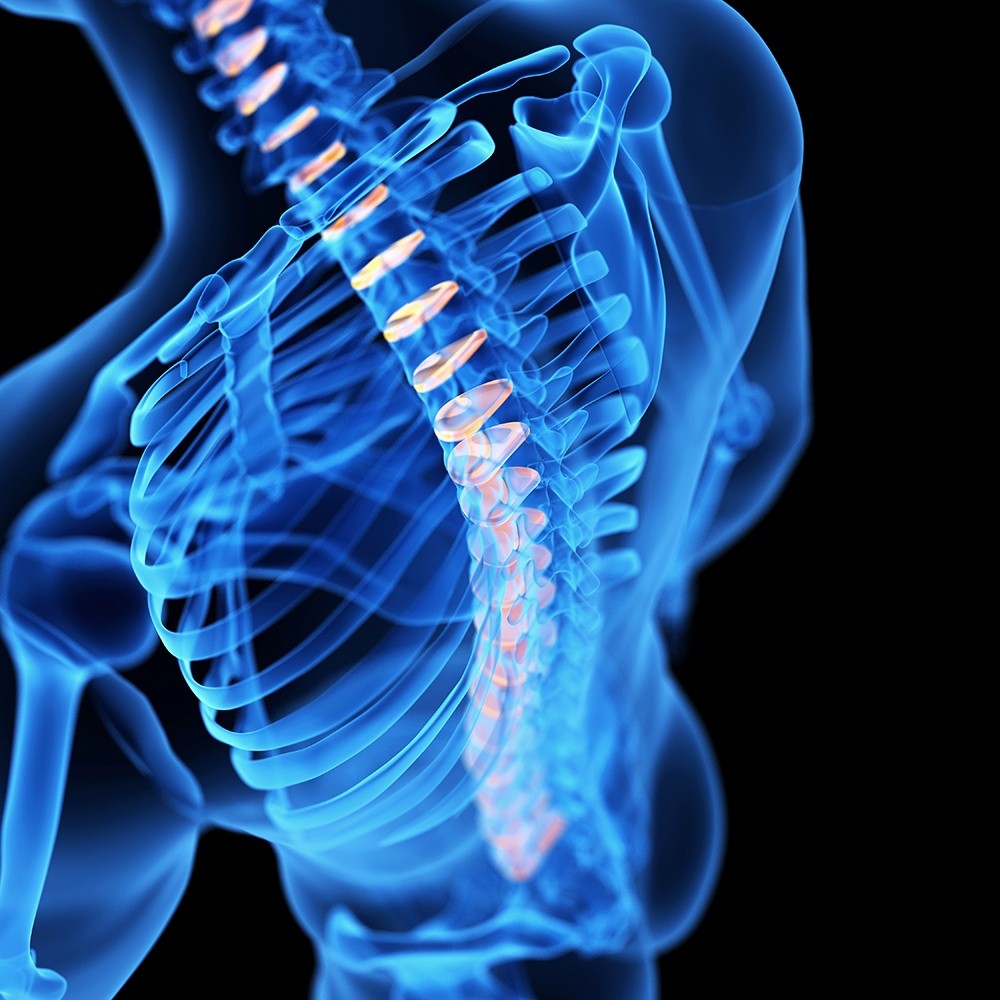
How Is Neoplastic Meningitis Diagnosed?
An MRI (magnetic resonance imaging) with enhanced contrast dye such as gadolinium-based, may show the presence of neoplastic meningitis. A lumbar puncture, or spinal tap, is used to draw out a portion of cerebrospinal fluid (CSF). Although the needle is inserted close to where the neoplasm is expected to be, often several draws are needed to increase the likelihood of verifying whether cancer cells are present in the CSF. A CSF flow study will also show blockages or collections of fluid.
State-of-the-Art Treatments for Neoplastic Meningitis at NSPC
Neoplastic meningitis treatments are considered palliative, with an emphasis on limiting symptoms such as neurologic deterioration and extending quality of life. NSPC Brain & Spine Surgery (NSPC) (NSPC) is at the forefront of advanced brain cancer treatments and participates in clinical trials to help in the search for cures to these life-changing cancers.
Chemotherapy
The blood-brain barrier hampers toxins, viruses and bacteria from permeating the brain’s tissues. However, this same blood-brain barrier also hinders most cancer-fighting drugs from reaching these tissues. Administering intrathecal cancer drugs directly into the cerebrospinal fluid (CSF), helps bypass the blood-brain barrier.
Chemotherapy can be delivered directly to the CSF via a lumbar puncture or Ommaya reservoir. A neurosurgeon places an Ommaya reservoir—a small bubble-shaped basin created just under the scalp with an attached tube that drains directly into one of the ventricles of the brain—during a craniotomy to allow chemotherapy to easily reach the meninges.
Stereotactic Radiosurgery
NSPC’s skilled neurosurgeons use image-guided stereotactic radiosurgery, such as Gamma Knife® or CyberKnife®, as an alternative to whole-brain radiation. Stereotactic radiotherapy can precisely target tumors or other malignant growths while preserving the nearby tissue. The treatment is bloodless and often completed in one single session.
NSPC consists of a multidisciplinary team of board-certified neurosurgeons and convenient offices on Long Island and the NYC area. NSPC’s award-winning doctors are leaders in the New York medical community, and many serve as chiefs of neurosurgery in NY hospitals. These expert physicians specialize in a range of neurosurgical subspecialties and related fields such as interventional neuroradiology, neuro-oncology, epileptology (epilepsy neurology), neurophysiology, critical neurology and pain management.

Related NSPC Center
Long Island Brain and Spine Tumor Center
NSPC provides state-of-the-art treatment of benign and malignant brain and spine tumors, using minimally invasive procedures like Gamma Knife®, Novalis TX™, and CyberKnife® rather than major surgery whenever appropriate. Our physicians also perform experienced pediatric neurosurgery — they give personalized, individual attention combined with knowledge and experience to take on the most challenging of cases.
Connect With Our 7 Convenient Locations
across Long Island, NY
Our expert physicians, surgeons and doctors are ready to serve you at our 7 convenient locations across Long Island, NY. Connect today to learn how our award winning, world class experts can help.
4250 Hempstead Turnpike Suite 4,
Bethpage, NY 11714
(516) 605-2720
COMMACK
353 Veterans Memorial Hwy,
Commack, NY 11725
(631) 864-3900
One Hollow Lane, Suite 212
Lake Success, NY 11042
(516) 442-2250
MANHATTAN
215 E. 77th Street Ground Floor
New York, NY 10075
(646) 809-4719
EAST SETAUKET
226 North Belle Mead Road, Suite C
East Setauket, NY 11733
(631) 828-3001
100 Merrick Road, Suite 128W
Rockville Centre, NY 11570
(516) 255-9031
WEST ISLIP
500 Montauk Hwy
West Islip, NY 11795
(631) 983-8400
World
Class
Expertise
For over 50 years & 350,000 patients NSPC has been a trusted global medical leader.
Contact us today for an appointment or consultation.
